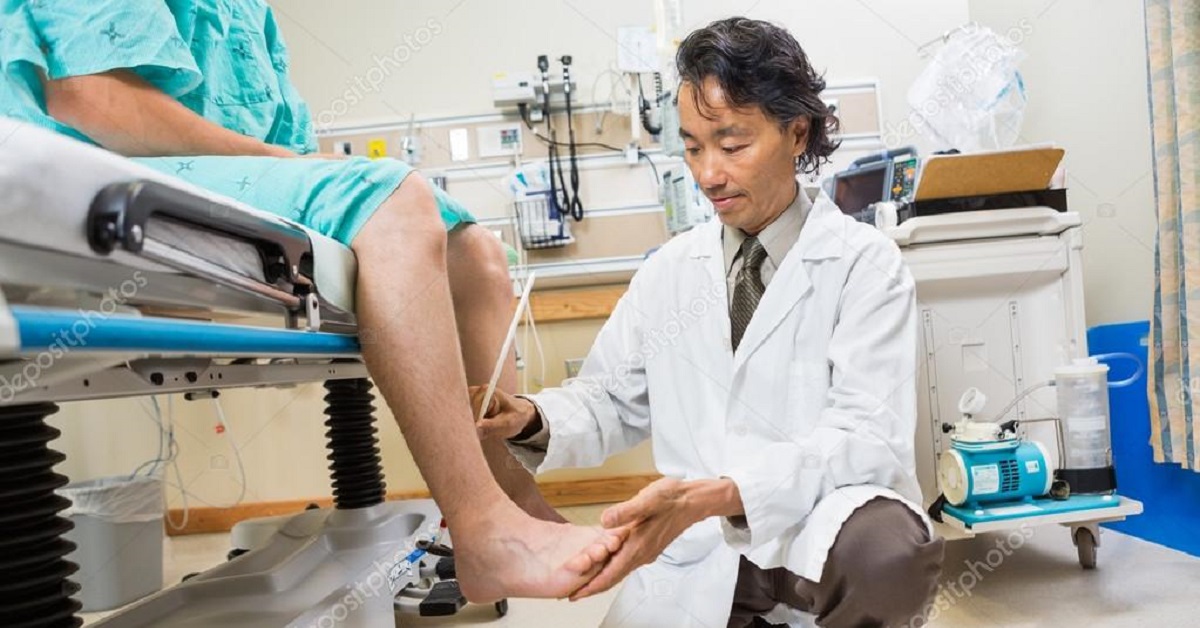
A simple test carried out at the doctor’s office compares blood pressure in the ankle to the pressure at the brachial artery in the upper arm. It’s called the Ankle Brachial Index (ABI).
Doctors use it to determine whether a patient suffers from peripheral artery disease (PAD), a condition that causes reduced blood flow to the legs.
But in recent years, doctors began using the ABI test to diagnose more than just PAD. They believe that poor test results may be an indicator that cognitive decline and dementia looms on a patient’s horizon. Let’s see how this new discovery can help you get a clearer picture of your brain health.
Understanding Ankle Brachial Index
Narrowing of the blood vessels in the lower extremities becomes more prevalent with age, affecting ten percent of people over age 65 and 20 percent of those beyond age 80. This narrowing reduces arterial blood flow to the lower limbs, a condition called peripheral artery disease (PAD). PAD often causes a painful ache in the legs when walking. Diabetes is a common cause of PAD, although not the only one.
A normal reading on the ankle brachial index, or ABI test, ranges from 1.0 to 1.4, showing modestly higher pressure in the ankle compared to the arm.
An ABI a little below 0.9 indicates some limited narrowing of the arteries caused by plaque buildup. A reading below 0.8 is considered moderate PAD. PAD becomes severe when the ABI drops below 0.5.
Now, what do these results mean to your memory?
Lower ABI is a Predictor of Lower Cognition
The first important study to reveal that a low ABI reading is a predictor of cognitive decline occurred at the University of Edinburgh, Scotland in 2006.
The researchers enrolled 717 men and women ages 55 to 74, and found that a lower ABI at the start of the study was linked to lower scores on non-verbal reasoning, processing speed and verbal fluency ten years later.
In 2011, researchers in France conducted a review of 12 studies. In all but one, researchers found a significant link between a low ABI (below 0.9) and future cognitive impairment, dementia or Alzheimer’s.
Results Confirmed in a Lifelong Study
Before 2014, researchers cited a major limitation of previous studies, pointing to the fact that information about the study participants’ early education was not available. This is important, because lower cognitive functioning in childhood is linked to heart disease and vascular dementia later in life.
So, the University of Edinburgh carried out a new study that analyzed data collected from the Lothian Birth Cohort, made up of participants born in either 1921 or 1936, which included results of IQ tests starting at the age of 11.
Throughout the years, members of the Lothian Birth Cohort underwent a barrage of cognitive tests, lifestyle questionnaires, medical examinations, blood tests and brain scans.
The new investigation included 918 dementia-free participants from the cohort who were in their 70s and 80s. The research team found – after taking into account many variables including childhood mental ability – that those with a lower ABI had worse cognitive performance in their senior years, most consistently struggling with mental processing speed.
Researchers explained their findings saying, “These results indicate that PAD is associated with impairment of cognitive function in relatively healthy older adults, free of stroke and symptomatic cardiovascular disease.”
What Happens During an ABI Test?
An ABI test takes only about ten or 15 minutes. It involves a cuff wrapped around your arm to take your blood pressure. Then your doctor uses a Doppler ultrasound to listen to your blood flow. To use this device, your doctor puts a dab of gel on your arm just below the blood pressure cuff and then applies the ultrasound.
Next, they’ll follow the same steps on your other arm, and then on both of your ankles. If your doctor is trying to confirm a diagnosis of PAD, he or she might take two ABI readings, one before you walk on a treadmill and one after.
A Valuable Early Warning Indicator
Since the ABI test is an easily applied, low cost measure with no risk to the patient, memory researchers believe it would be a clinically useful tool to provide early detection and intervention in people at high risk for cognitive decline.
The major cardiovascular societies advise an ABI measurement in every smoker and diabetic over 50 years of age, and everyone else over age 70.
But considering that PAD can build up over a lifetime, and symptoms may not become obvious until the artery has narrowed by 60 percent or more, it would make more sense for physicians to carry out an ABI for all their patients, starting well below the age of 70.
In my opinion, the earlier you can determine you’re on the path to cognitive decline, the sooner you can make changes in lifestyle that can protect your brain and preserve your memories. In fact, I think that would be a fascinating study to carry out to investigate the benefits of lifestyle change in the prevention of dementia.
Let’s examine folks with a low ABI in mid-life, and those willing to adopt positive lifestyle changes over the years that follow, then let’s examine them again in their 70s, 80s and even their 90s. I have a hunch the research would show a smaller decline in ABI, and that many of these people will prove able to stave off cognitive decline.