Rogue proteins called amyloid beta and tau are often named as the hallmarks of Alzheimer’s disease. If you’ve been around the dementia biz for more than a week you’ve heard about amyloid beta and tau over and over.
It’s these proteins that form the famous plaques and tangles in the brain. These sticky clumps and twisted fibers lead to cell death, memory loss and brain damage.
But there are some people whose brains are riddled with amyloid and tau, yet show no signs of dementia. How can that be?
Could scientists be on the wrong track in their attempt to design drugs that target these plaques and tangles?
Increased Blood Flow Compensates for Brain Plaques
A 2013 review covered studies of adults who have amyloid brain deposits, but enjoy good mental health all the same. The authors concluded that. . .
- Up to one in three older people with normal thinking ability have brain plaques
- A significant increase in these plaques is detectable in cognitively normal people as time goes by
- The size and existence of these plaques does not correlate well with cognitive performance or brain volume
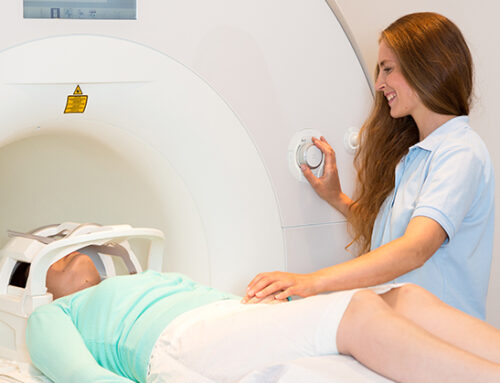
In 2014, researchers working at the University of California, Berkeley, scanned the brains of 71 adults of varying age who had good cognition and memory. 16 of the older members of the group had evidence of amyloid.
The participants were asked to memorize a number of photographs and were questioned about what they saw.
The researchers found those with amyloid plaques had increased blood flow and stronger activation of brain regions associated with memory. They were able to ramp up brain activity to compensate for the plaques.
Research presented at the Society for Neuroscience 2016 Annual Conference in November raises further doubts about the importance of these plaques.
“This is Amazing”
Eight people over the age of 90 were found to have superior performance — as good as people 40 years younger — on memory and cognition tests, right up until the day they died.
Yet autopsy findings revealed widespread plaques and tangles. In three of the eight, the damage was so severe, if the researchers not been aware of their backgrounds they would have diagnosed those people with full-blown Alzheimer’s.
Lead investigator Changiz Geula, research professor at the Cognitive Neurology and Alzheimer’s Disease Center at Northwestern University, Chicago, said, “This is amazing. We never expected it.”
In examining the hippocampus, a key area for memory, they found the nerve cells were pretty much intact, a surprising finding, because plaques are considered toxic and should lead to the death of neurons.
Another member of the research team, Dr. Aras Rezvanian, said “The oldest old with superior memory can display the full range of Alzheimer’s pathology. It points to some unknown factors that protect some elderly…”
Another Drug Trial Ends in Failure
The decade up to 2012 saw the failure of 243 out of 244 drugs for treating Alzheimer’s. Even the one that was successful had little impact.
In November, a clinical trial for solanezumab, a drug which directly targets beta amyloid, ended in failure.
Dr. Reisa Sperling, professor of Neurology at Harvard Medical School, who leads a separate trial on solanezumab, said she still believed in amyloid as a principal factor in Alzheimer’s development.
I guess she’s still hoping the amyloid-busting drug will work out.
I think she and like-minded researchers are on the wrong track.
While there’s little doubt that amyloid and tau play some role in Alzheimer’s pathology, drugs that merely target these proteins without taking account of innumerable other factors are likely to meet with the same fate as all the other failed pharmaceuticals.
In our video summit last fall, Awakening from Alzheimer’s, we interviewed 14 doctors and academic researchers on the cutting edge of brain and memory research. Several of them mentioned that the focus on brain plaques is misguided.
Brain plaques are most likely a symptom of inflammation. In effect, the body’s tissue – whether it’s the lining of your arteries or your brain – lays down a coating of fats or proteins to protect itself against the assault of inflammatory molecules like COX-1, COX-2 or IL6 (there are many such molecules).
If this theory is true – and I believe it is – then we need to treat inflammation, not look for drugs to get rid of brain plaques. It’s quite likely the brain plaque theory of Alzheimer’s disease will go the way of the cholesterol theory of heart disease. The plaques are the symptom, not the cause.
There is an epidemic of chronic inflammation in our society that is linked to heart disease and dementia as well as arthritis, cancer, and more.
Why are we so inflamed? The leading reason is probably high blood sugar, leading to metabolic syndrome (basically, prediabetes), and to full-blown diabetes.
This is a big subject, but if you’re not minding your blood sugar (and if you’re overweight, you probably aren’t) then I recommend our book Defeat High Blood Sugar.
I know it’s hard for people to change the way they eat, and to lose weight. That’s why our book focuses on nutrients and supplements that get blood sugar under control without calorie counting.