When it comes to treating somebody who is just beginning to suffer Alzheimer’s disease, the conventional medicine folks have a big problem.
They don’t know how the disease starts. So they can’t catch it at an early stage. In fact, 20 years ago when my mother was developing dementia, her doctor didn’t know a thing about it.
Awareness is much higher now, but a doctor still can’t diagnose the condition until memory gaps become so big they can’t be overlooked. And that seems to happen only after extensive damage has already taken place in brain tissue.
What to do? Researchers have made some promising new findings about early-stage Alzheimer’s. . .
Scientists at the Washington University School of Medicine in St. Louis think they’ve found the answer to what happens in the early phases of Alzheimer’s disease. They say it’s linked to the behavior of the brain’s microglia – immune cells that roam the brain to help protect its neurons and keep them in good working order.
According to the Washington U. team, microglia sometimes follow a crucial pattern of activity that allows Alzheimer’s destruction to flow through neurons. Correct that activity – and there are natural ways to nudge it in the right direction – and you may stop Alzheimer’s before it becomes a serious problem.
Plaque Attack!
In the tests conducted by the Washington U. researchers on people and animals, they found that two kinds of damaging proteins begin to collect in the brain years before a person begins to show memory loss.
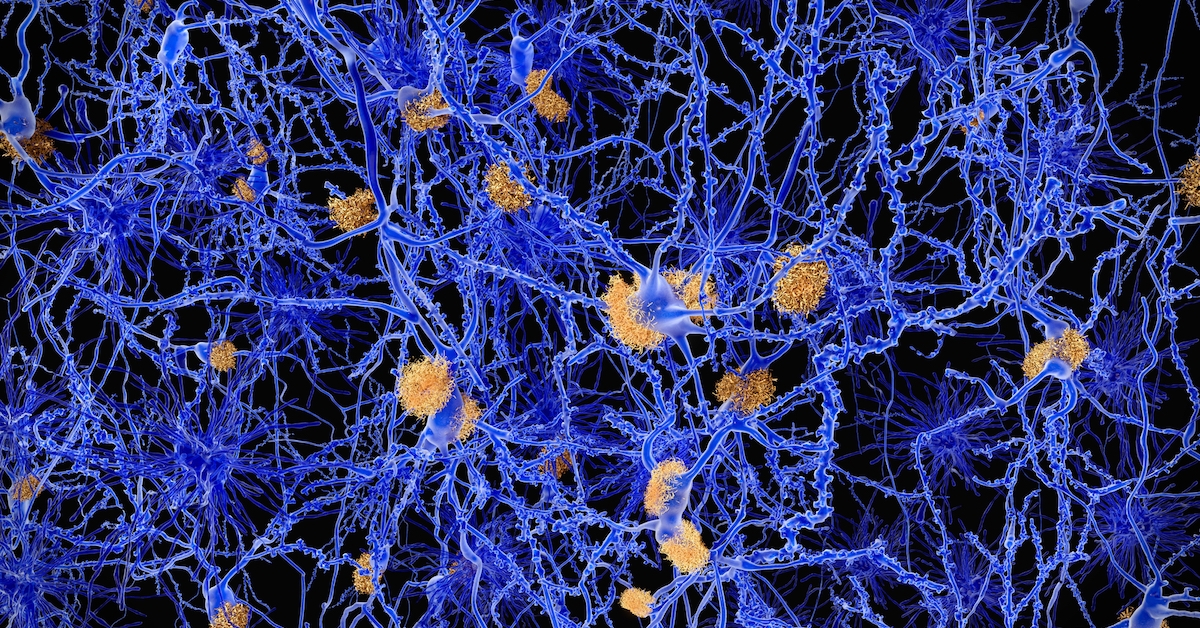
You won’t be surprised to hear these compounds are amyloid beta (which forms plaque) and tau (which forms tangles). Of these two, say the scientists, the tau is particularly destructive. When the tau proteins overwhelm neurons, the nerve cells start to die off. And that sets off the memory erasure and disorientation that are characteristic of Alzheimer’s disease.
The scientists note that plaque comes first, and that if the immune response by microglia can seal off the plaque, serious damage to the brain can be curtailed. But if these cells fail to keep the amyloid plaque quarantined, the resulting damage to neurons leads to toxic results in the brain tissue. Then, that toxic spillover spurs on the formation and spread of tau’s memory-cancelling tangles.
“I think we’ve found a potential link between amyloid and tau that people have been looking for for a long time,” says researcher David Holtzman. “If you could break that link in people who have amyloid deposition but are still cognitively healthy, you might be able to stop disease progression before people develop problems with thinking and memory.”
This tallies with what I’ve seen elsewhere – that tau seems to play a bigger role in Alzheimer’s than amyloid beta. And perhaps it accounts for why plaque-busting drugs from Big Pharma have failed so badly. A wide body of evidence suggests that plaques are not the smoking gun when it comes to dementia.
Holes in the Amyloid Beta Theory
Dr. Holtzman and his colleagues point out that amyloid plaques by themselves do not cause Alzheimer’s and other forms of dementia. Many folks in their 70s who have amyloid plaques don’t experience any loss of memory or cognition. Long-time readers of this newsletter already know this.
What’s new here is that when amyloid plaques result in tau tangles, it DOES appear to lead to Alzheimer’s.
Now I won’t pretend there are any sure-fire ways to improve how your microglia behave. But research does point toward lifestyle measures that might help these immune cells to continue doing their jobs and thereby lower your risk of memory issues.
Making Microglia More Effective
The first measure is to get enough sleep. Research in Asia shows that when you miss out on sleep, your microglia change their function.1 This research, conducted on animals, mainly focused on how lack of sleep influences the ways microglia maintain the health of the synapses that link neurons together in the brain. While the scientists found larger effects during adolescence, their results showed that lack of sleep at any age “adversely affected short-term memory.”
Meanwhile a study at the Georgia Institute of Technology shows that getting too little sleep and not consistently going to bed at the same time each night makes it harder for older people to recall recent events in their lives.2
Another way to help out your microglia is to get more quercetin in your diet. Research shows this nutrient – a pigment found in foods like cherries, berries, apples, broccoli and onions – can protect microglia from oxidative damage.3 (Quercetin is also available as a supplement.)
And tests at Johns Hopkins, also on animals, show that quercetin can be part of a program that lowers the risk of Alzheimer’s disease.4 Human studies will be required before the medical community accepts these findings (assuming they do so even then, considering it won’t lead to a new drug.)
Added to all of this, as I never tire of saying, go out and do some walking or get some other form of exercise. Researchers at Texas Christian University have found evidence that exercise may be a way to encourage microglia to clear misfolded proteins out of the brain and improve brain function.5