While the vast majority of scientists focus their Alzheimer’s research efforts on banishing plaque from the brain, others are looking at different ways to prevent and reverse dementia.
One alternative is to target another factor linked to the disease — brain inflammation.
By stopping inflammation in its tracks, scientists found they were able to reverse dementia in mice. Now they’re optimistic this strategy will work in humans, too.
Your brain has a natural protective mechanism to prevent damage to brain cells and neurons that control thought and other important processes in your body. It’s called the blood-brain barrier (BBB), and it separates the blood circulating through your body from your brain.
The BBB allows nutrients and other healthy molecules to pass through into the brain but keeps out molecules perceived as a threat.
Unfortunately, by age 70 almost six out of ten people will have a leaky blood-brain barrier allowing potentially harmful molecules to enter. This is thought to contribute to some of the decline in mental function that comes with aging.
One of these negative molecules appears to be the protein albumin.
Inflammatory Protein Triggers Brain Aging, Memory Loss
In laboratory study, researchers found that a leaky BBB allows albumin to gain entry to brain tissue. Albumin binds to a receptor called TGF-beta in a type of brain cell called an astrocyte. This leads to a cascade of inflammatory events that disrupt brain rhythm and create dysfunction in the hippocampus, a key center for memory and learning.
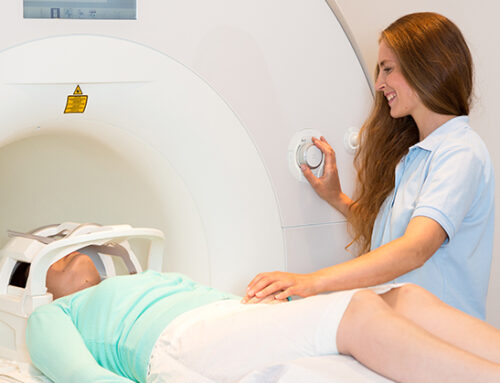
The same brain wave disruption is seen in EEGs of people who suffer with Alzheimer’s, mild cognitive impairment and epilepsy. Scientists confirmed these findings by using an advanced MRI scanning technique. The scans revealed that the more extensive the leakage in the BBB, the greater the decline in cognition.
In the latest experiments published in two papers in the journal Science Translational Medicine in December, a 27-strong team of scientists led by the University of California, Berkeley, introduced albumin into the brains of young mice. Within a week their brains looked like those of elderly mice and they performed just as poorly as their seniors in a maze test.
Then the researchers used mice genetically engineered to knock out the TGF-beta receptor in old age so albumin can’t bind to it. Their senile brains looked youthful again and performed as well as young mice in the maze test.
Next they gave old mice a drug called IPW that lowered the receptors’ activity to levels seen in those of young mice. Now their brains looked younger, displayed youthful brain-like gene expression, had lower levels of inflammation, improved brain rhythms, and were less susceptible to seizures. The aged mice were also able to navigate a maze just as well as the young ones.
Finally, in analyzing human brain tissue they found evidence of albumin in older brains. In addition, they found increased levels of TGF-beta and greater inflammation in older brains.
Remove Inflammation – “Reverse Brain Aging”
Daniela Kaufer, a UC Berkeley professor of integrative biology and senior author of the experiments, said, “Age involves loss of function and dead cells. But our new data tell a different story about why the aged brain is not functioning well: It is because of this ‘fog’ of inflammatory load.
“But when you remove that inflammatory fog, within days the aged brain acts like a young brain. It is a really optimistic finding in terms of the capacity for plasticity that exists in the brain. We can reverse brain aging.
“This is new biology, a completely new angle on why neurological function deteriorates as the brain ages.”
Professor Kaufer believes that since a leaky BBB can be detected by MRI and an EEG can detect abnormal brain rhythms, these allow doctors to flag people at risk. There’s also the potential of a drug to slow or reverse these problems.
“We now have two biomarkers that tell you exactly where the blood-brain barrier is leaking, so you can select patients for treatment and make decisions about how long you give the drug,” she said.
“You can follow them, and when the blood-brain barrier is healed, you no longer need the drug.”
Experts asked to comment on these studies were positive but cautious. “These two exciting reports highlight the ability of transient inflammation-related changes to alter cognitive function,” says Diego Gomez-Nicola, Associate Professor in Neuroscience, University of Southampton, England.
“This work is important, as it demonstrates transient changes to the permeability of the blood-brain barrier in dementia, and how these drive local changes in the brain. However, the interpretations of this study must be raised with caution, as mostly relying on data from mouse models.”
The drug interventions the researchers predict are years in the future (if ever). Meanwhile, reduce inflammation throughout your body any way you can: An anti-inflammatory diet, adequate sleep, and anti-inflammatory supplements such as turmeric, boswellia, silymarin, and proteolytic (protein-eating) enzymes such as bromelain and papain.
I don’t have information at my fingertips as to which of these nutrients might penetrate the blood-brain barrier – that’s a whole topic in itself. But they do reduce system-wide inflammation and they are completely safe.