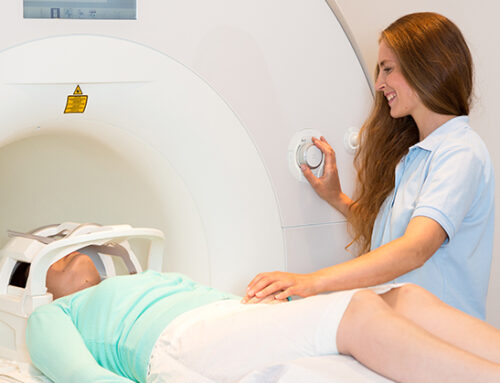
In breakthrough research, scientists have, for the first time, diagnosed a neurodegenerative condition in living patients using a non-invasive technique. The condition, of course, is Alzheimer’s.
And unlike the blood tests that are under development to identify proteins linked to Alzheimer’s disease in a patient’s blood, this test relies on a beam of light and a computer.
In addition, it’s far cheaper, less complex, and less hazardous than “gold standard” brain scans and spinal taps that are in use in hospitals across the country. Here are the remarkable details…
Currently, the best diagnostic methods available for testing whether someone has Alzheimer’s disease are usually employed after symptoms of memory loss appear. They do little to nothing to help doctors and patients detect Alzheimer’s disease in its earliest stages.
What’s more, the only way Alzheimer’s can be diagnosed with certainty is after death, during autopsy.
This is clearly unacceptable, so scientists at the Veterans Administration Bedford Healthcare System in Eastern Massachusetts have been working on a new diagnostic test.
They developed a visual technique that makes use of spectroscopy, a machine that measures how light moves through and bounces off matter. In the process, the scientists made a fascinating discovery…
Diseased and Healthy Tissues Reflect Different Wavelengths of Light
Depending on the type of material the light is targeted at, and the wavelengths of light energy it generates, the energy will be blocked to some extent, causing it to be absorbed into the material or scattered back.
For brain analysis, two fiber optic probes are positioned on the temples. The source probe delivers near-infrared light. This type of light penetrates deep into the brain. The other probe collects the light that bounces back.
The returning light will act differently after it has reacted with the brain tissue and this difference in light refraction can be measured. Since those with Alzheimer’s will have chemical and structural changes in brain tissue that differentiate diseased brain tissue from healthy brain tissue, spectroscopy has the potential to be a very useful diagnostic tool.
To test this, the researchers first used autopsy samples from people both with Alzheimer’s and those without the disease. The technique was successful in distinguishing Alzheimer’s brain tissue from healthy brain tissue. What’s more, the researchers were able to identify refraction characteristics of the diseased tissue.
Next they tested the new technique in living people.
Identified Severity of Mild Cognitive Impairment
A small number of healthy volunteers, those with mild cognitive impairment (MCI), and late-stage Alzheimer’s patients – later confirmed at autopsy – were enrolled.
The research team devised a computer algorithm to identify patterns in the spectroscopy data and were able to distinguish between Alzheimer’s patients and healthy controls.
Further adjustments allowed them to classify patients with MCI according to degrees of impairment. For example, one spectral feature might allow for early Alzheimer’s diagnosis while another may document disease progress in an already diagnosed case.
Lead researcher Dr. Eugene Hanlon explains, saying, “This technology is significant because it probes the biochemical and cellular structures of the brain non-invasively with a technique that is inexpensive and could be put into widespread use.
“Most importantly, it gives useful information about those with mild cognitive impairment.”
First author, Frank Greco, believes veterans, especially, could be helped. “Veterans are more at risk for Alzheimer’s than the general population,” he explains. “This technique has the potential to help identify what factors may increase that risk.”
A much larger study is needed to confirm the usefulness of the tool but the researchers are optimistic it will be successful. “If so,” the authors write, “this approach could become a safe, non-invasive method for assessing response to treatments in real time.”